Le Infezioni in Medicina, n. 3, 329-332, 2025
doi: 10.53854/liim-3303-10
CASE REPORTS
A destruent case of recurrent primary naso-pharyngeal tuberculosis in a migrant
Andrea Sergio Sarassi1,2,3, Niccolò Riccardi3,4, Giovanni Fumagalli1,3,4, Alessandra Pelosi5, Alice Claudia Repossi3,4, Maurizio Ferrarese3,4, Marco Mantero1,2, Francesco Bruno Arturo Blasi1,2, Luigi Ruffo Codecasa3,4
1Department of Pathophysiology and Transplantation, University of Milan, Milan, Italy;
2Respiratory Unit and Cystic Fibrosis Center, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Milan, Italy;
3StopTB Italia ODV, Milan, Italy;
4Regional TB Reference Centre and Laboratory, Villa Marelli Institute, ASST Grande Ospedale Metropolitano Niguarda, Milan, Italy;
5Dermatology Outpatients Unit, Villa Marelli Institute, ASST Grande Ospedale Metropolitano Niguarda, Milan, Italy.
Article received 20 April 2025 and accepted 10 June 2025
Corresponding author
Andrea Sergio Sarassi
E-mail: andrea.sarassi@unimi.it
SummaRY
A 24-year-old Ukrainian man with post-natal developmental disability was treated for presumptive facial cutaneous TB in 2018 in his home country. After moving to Italy, his nostril lesion recurred in 2021, expanding to the upper lip, but he was lost to follow-up before a diagnosis was made. In 2023, when symptoms worsened, a biopsy was performed showing chronic inflammation and negative microbiological molecular tests and culture. By 2024, the lesion spread to the eyelids with worsening ulcerations. After surgical resection, histology revealed a vegetative, haemorrhagic mucosa with necrotic granulomatous inflammation and rifampin-susceptible Mycobacterium tuberculosis (Mtb) was detected at molecular testing. Diagnosis of recurrent primary cutaneous TB without pulmonary involvement was made and treatment for drug susceptible TB was initiated, leading to complete remission of the facial lesions.
Primary cutaneous TB without pulmonary involvement is rare, presenting as nodules, plaques, papules, or ulcers. Diagnosis requires systemic evaluation, imaging, infection screening and expert consultation. Cutaneous TB (CTB) is uncommon in Ukraine and accounts for less than 2% of extrapulmonary TB cases with frequent association with immunosuppression and delayed presentation. Although infrequent, CTB mirrors the wider TB scenario, that is also characterized by MDR-TB in 27% of new and 45% of retreatment cases, and XDR-TB in 13% of MDR-TB cases. In individuals coming from TB endemic areas with strong clinical suspicion, empirical TB diagnosis should always be considered despite negative microbiology to enable timely treatment and prevent progression. A multidisciplinary approach is essential for accurate diagnosis and optimal management.
Keywords: primary cutaneous tuberculosis, recurrent skin lesions, TB, endemic countries.
INTRODUCTION
Cutaneous TB (CTB) is a rare extrapulmonary form of Mycobacterium tuberculosis (Mtb) infection and accounts for less than 2% of all cases of tuberculosis (TB) worldwide [1]. Its presentation is varied and tends to mimic other infections as well as neoplastic skin diseases, thus delaying correct diagnosis if not promptly suspected [2]. CTB can occur through direct inoculation, contiguous extension, or via hematogenous spread and is more common in immunocompromised patients and in those from areas with high-endemic rates [3]. In countries with high TB burdens such as East Europe (e.g. Ukraine), empirical anti-tubercular management is common even without any confirmatory microbiological evidence upon presentation [4].
Reactivation of CTB years after the establishment of clinical remission is uncommon and represents further diagnostic dilemmas. When the lesions of CTB are extended (e.g. facial, mucosal, and periocular areas) should be fully evaluated and managed with a multidisciplinary team to reduce functional and cosmetic consequences [5].
CASE REPORT
In 2018, a 24-years old man, born in Ukraine, developed a cutaneous lesion of the left nostril. The patient was affected by severe motor and cognitive impairment as result of anoxic damage at birth. The illness was treated in the country of origin as presumptive Tuberculosis (TB), in absence of definitive microbiological confirmation, with subsequent clinical remission. The patient moved to Italy in 2020. He was in apparent good health until 2021, when recurrence of the cutaneous lesion at the same site occurred. The patient was referred to the dermatology Unit of our Hospital for comprehensive diagnostic assessment.
Unlike the first episode, the lesion showed a progressive expansion towards the upper lip. Dermatological examination was inconclusive and the patient was advised to undergo periodic outpatient follow-up. However, the patient was lost to follow up until march 2023, when he presented once again at the Dermatology Unit for worsening of the lesion. Blood tests, such as C-reactive protein (CRP), procalcitonin, full blood count, liver and renal function tests, electrolytes, were within the normal value. Subsequently, Chest and spinal X-ray were performed and returned negative. A CT scan of facial bones was performed, without evidence of bone necrosis. Then, an incisional biopsy of the lesion showed both active and chronic inflammation with giant cell reaction. Molecular and cultural analysis of the surgical specimens were negative for Mycobacterium tuberculosis (Mtb) bacteria and parasites. HIV serology resulted negative. Dermatological suspicion was balancing between cutaneous TB and leishmaniasis; however, in absence of a confirmed diagnosis, specific antimicrobial therapy was withheld, and close follow-up was carried on.
In March 2024, the patient was referred to our Hospital for further worsening of the clinical presentation. At clinical examination, compared to 12 months earlier, the formation on the upper lip progressively grew in size, and the areas of ulceration and exudation worsened significantly. Moreover, similar lesions appeared on the homolateral upper and lower eyelids (Figure 1, panel A). However, ophthalmological, dermatological and ENT visits were inconclusive. Intraoral examination was further complicated by the prior extensive dental pathology affecting both arches. A suspected discontinuity of the hard palate was noted, apparently not visible at the CT scan of March 2023. Consequently, the patient was hospitalized to perform surgical resections of the lesions. At histology, pharyngeal mucosa presented a vegetative and haemorrhagic appearance, with necrotic granulomatous inflammation. Serological and histological analysis were negative for leishmaniosis. Mtb was detected through polymerase chain reaction (PCR) in the biotic sample (GeneXpert) without rpoB resistance, while culture grew drug-susceptible Mtb. A four drug induction regimen with isoniazid, rifampin, pyrazinamide and ethambutol was started for two months, followed by maintenance treatment with isoniazid and rifampin for the following seven months. Skin lesions positively responded to therapy with complete remission (Figure 1, panel B).
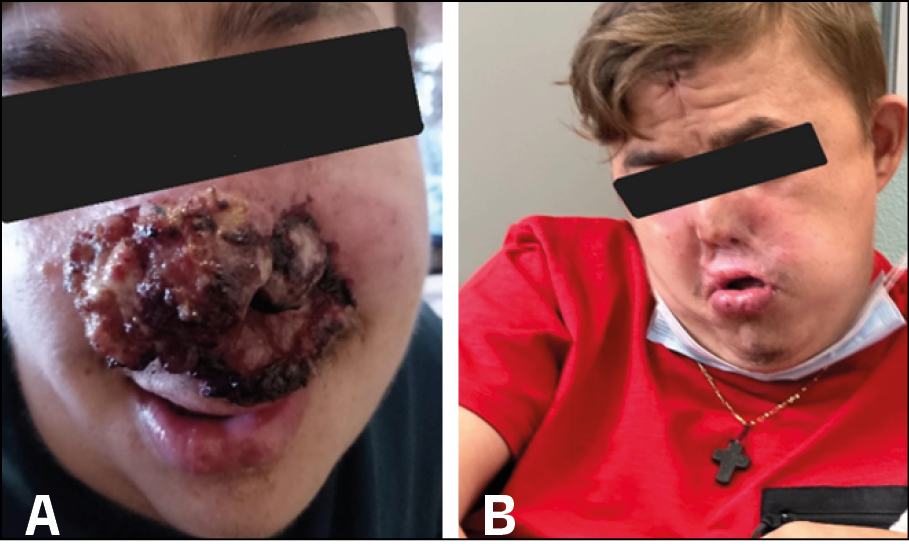
Figure 1 - Panel A: nasal tip was deformed from atrophic and retracting scars, as result of recurrent ulcerative-exudative phenomena. Moreover, the upper lip was disrupted, being enlarged, and thinner, with intact skin, except for the labiogenial margins, showing ulcerative-exudative lesions with serous-crusted material. Similar structural alteration was observed in the homolateral upper and lower eyelids, appearing replaced by inflammatory tissue, with a mamillated and exudative appearance.
Panel B: clinical presentation after 9 months of antitubercolar treatment ( 2 months HRZE, 7 months HR).
DISCUSSION
Primary cutaneous TB, without pulmonary involvement, is uncommon and it may present as nodules, рlаques, papules and chronic ulcers [6]. It is classically divided into true cutaneous TB and tuberculids. The former is characterized by the presence of mycobacteria at skin site, while the latter are sterile lesions resulting from hypersensitivity reaction to mycobacterial antigens [7]. A careful evaluation for systemic involvement, chest X-ray, thorough medical history and screening for other cutaneous infectious diseases and HIV should always be performed [8]. Among the possible aetiologies of exudative and ulcerating cutaneous skin lesions, malignant, inflammatory and infectious diseases should be all included [9]. Malignancies include squamous cell carcinoma and malignant melanoma; the latter may present as an ulcerative lesion, mainly associated with the nodular type, the most aggressive form of melanoma. On the other hand, inflammatory disorders of the skin list discoid lupus erythematosus (LE), cutaneous sarcoidosis and discoid eczema [10]. Among infectious skin diseases in migrants from TB endemic areas, Lupus vulgaris, a rare chronic form of cutaneous TB, ecthyma gangrenosum (EG) and, less commonly, tinea faciei should be considered [11]. CTB shares also clinical features with leishmaniasis, tertiary syphilis, and deep mycoses, often presenting as ulcerative or granulomatous lesions, complicating diagnosis. In endemic or re-emerging areas, such as northern Italy for leishmaniasis [12], and in atypical syphilis presentations [13], thorough differential diagnosis is critical. Histopathology, supported by specific molecular or serological tests, remains essential for distinguishing CTB from deep fungal infections [14].
Literature reports few cases of primary nasopharyngeal and cutaneous TB, usually with favourable outcome, regardless of disease extension [15-20].
In Italy, TB is increasingly rare, with CTB being even more uncommon. As a result, limited clinical experience may contribute to delayed diagnoses. CTB is uncommon also in Ukraine, occurring in fewer than 2% of extrapulmonary cases; while TB prevalence remains high with drug-resistant (DR)TB diagnosed in 27% of new and 45% of re-treatment cases and extensively drug resistant (XDR)-TB in 13% of DR-TB cases [21, 22]. Health system disruptions and the ongoing conflict have further made TB control more difficult [23, 24].
In the case at hand, despite the patient’s origin from a high-burden area and a personal history of cutaneous TB, the diagnosis was postponed for nearly three years due to repeatedly negative microbiological tests. This delay can be partially attributed to the paucibacillary nature of many extrapulmonary TB manifestations, which often makes microbiological confirmation challenging.
In individuals coming from high burden TB countries and with a strong clinical suspicion, an empirical diagnosis should always be considered, even in the absence of microbiological confirmation. This approach enables the prompt initiation of anti-tubercular therapy, which is crucial for improving clinical outcomes and preventing disease progression. Given the potential for diagnostic uncertainty, a comprehensive differential diagnosis should be systematically pursued. In such cases, a multidisciplinary approach involving specialists in infectious diseases, pulmonology, and dermatology is essential to ensure diagnostic accuracy and optimize patient management.
CONCLUSIONS
To prevent disease progression and complication, even in the presence of negative microbiology, case history and clinical suspicion should require multidisciplinary approach in order to prompt empirical TB diagnosis and treatment of skin lesions in subjects originating from TB endemic regions.
Consent from patient
Consent for the manuscript publication, information and images management was obtained from the patient and the mother.
Authors’ contributions
A.S.S, N.R, G.F, A.P, A.C.R, M.F and L.R.C. took care of the patient and gave final approval of the version to be submitted; M.M and F.A.B.B participated in drafting the article and gave final approval of the version to be submitted.
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
No funding for this paper were used.
Data availability statement
Data were generated at Regional TB Reference Centre and Laboratory, Villa Marelli Institute, ASST Grande Ospedale Metropolitano Niguarda and are available from the corresponding author AS.S on request.
Ethics approval
Ethical approval was not sought for the present study because the study at hand is a case report. Consent from the patient and mother was obtained.
- Kovalchuk A, Yukhymenko N, Savchuk O. Clinical and epidemiological characteristics of extrapulmonary tuberculosis in Ukraine. Tuberk Lung Dis. 2021; 99(4): 24-29.
- Barbagallo J, Tager P, Ingleton R, et al. Cutaneous tuberculosis: diagnosis and treatment. Am J Clin Dermatol. 2002; 3(5): 319-328.
- Bravo FG, Gotuzzo E. Cutaneous tuberculosis. Clin Dermatol. 2018; 36(4): 491-498.
- Misirovs R, Johnston L, Green R. Primary nasopharyngeal tuberculosis. BMJ Case Rep. 2022; 15(12): e251927.
- Santos JB, Figueiredo AR, Ferraz CES, et al. Cutaneous tuberculosis: epidemiologic, etiopathogenic and clinical aspects - part I. An Bras Dermatol. 2020; 95(5): 564-578.
- Chen Q, Chen W, Hao F. Cutaneous tuberculosis: A great imitator. Clin Dermatol. 2019; 37(3): 192-199.
- Kaul S, Kaur I, Mehta S, et al. Cutaneous tuberculosis. Part I: Pathogenesis, classification, and clinical features. J Am Acad Dermatol. 2023; 89(6): 1091-1103.
- Kaul S, Jakhar D, Mehta S, et al. Cutaneous tuberculosis. Part II: Complications, diagnostic workup, histopathologic features, and treatment. J Am Acad Dermatol. 2023; 89(6): 1107-1119.
- Burns T, Breathnach S, Cox N, et al. Rook’s textbook of dermatology. Vol 1. 7th ed. Oxford: Blackwell Science; 2004.
- Fitzpatrick JE, Morelli JG. Dermatology secrets plus. 4th ed. Philadelphia: Elsevier Mosby; 2011.
- European Centre for Disease Prevention and Control, WHO Regional Office for Europe. Tuberculosis surveillance and monitoring in Europe 2023 – 2021 data. Stockholm: ECDC and Copenhagen: WHO Europe; 2023.
- Todeschini R, Musti MA, Pandolfi P, et al. Re-emergence of human leishmaniasis in northern Italy, 2004 to 2022: a retrospective analysis. Euro Surveill. 2024; 29(4): 2300190.
- Ciccarese G, Facciorusso A, Mastrolonardo M, et al. Atypical manifestations of syphilis: a 10-year retrospective study. J Clin Med. 2024; 13(6): 1603.
- Dhar S, Pradhan S, Saha A, et al. Deep fungal infections of skin and role of histopathology in diagnosis. Indian J Dermatol. 2024; 69(6): 442-452.
- Ekambi Kotto R, Nkoro GA, Mendouga Menye CR, et al. Cutaneous tuberculosis and its pleomorphic presentations in HIV-negative patients: a case report. J Med Case Rep. 2025; 19: 90. https://doi.org/10.1186/s13256-024-04918-0.
- Kerstens J, Sadiq AM, Kini LC, et al. A unique case of cutaneous tuberculosis of the scalp with extensive intracranial invasion. Acta Neurol Belg. 2025. https://doi.org/10.1007/s13760-025-02730-1.
- Grupper M, Potasman I. When uncommon uncovers: mucosal tuberculosis in a medical tourist from Burundi. J Travel Med. 2012; 19(1): 54-56. https://doi.org/10.1111/j.1708-8305.2011.00559.x.
- Taylor AEM, Corris PA. Cutaneous tuberculosis in an immunocompromised host: an unusual clinical presentation. Br J Dermatol. 1995; 132(1): 155-156.
- Warin AP, Wilson Jones E. Cutaneous tuberculosis of the nose with unusual clinical and histological features. Br J Dermatol. 1976; 95(Suppl. 14): 15-16. https://doi.org/10.1111/j.1365-2133.1976.tb07885.x.
- Pashchenko O, Kravchenko T, Demchenko A. Cutaneous tuberculosis in immunocompromised patients: a retrospective study. Dermatol Rep. 2020; 12(2): 8592.
- World Health Organization. Global Tuberculosis Report 2023. Geneva: WHO; 2023. PMID: 37893822.
- Zignol M, Dean AS, Alikhanova N, et al. Population-based resistance of Mycobacterium tuberculosis isolates to pyrazinamide and fluoroquinolones. Lancet Infect Dis. 2022; 22(4): 537-547.
- Taylor J, Morozova O, Leshchinsky N, et al. The impact of war on tuberculosis in Ukraine: a call for action. Lancet Respir Med. 2023; 11(8): 687-689.
- Fumagalli G, Riccardi N, Catalano G, et al. TB anywhere, TB everywhere: the first case of pre-extensively drug resistant tuberculosis treated with BPaL in Italy. Microb Drug Resist. 2025; 31(1): 12-15.